Neuroplasticity, often described as the nervous system’s ability to adapt its structure and performance in response to external stimuli, learning, or injury, represents a core principle in contemporary neuroscience. For decades, researchers assumed that the human brain stopped developing after early development. However, ongoing research has confirmed that the brain retains the ability to create additional neural pathways throughout life. This dynamic feature allows the nervous system to restructure itself after damage caused by cerebrovascular events, traumatic brain injury, or chronic neurological conditions. Understanding neuroplasticity has become a primary priority in rehabilitation medicine because it provides a evidence-based foundation for functional restoration and measurable improvement.
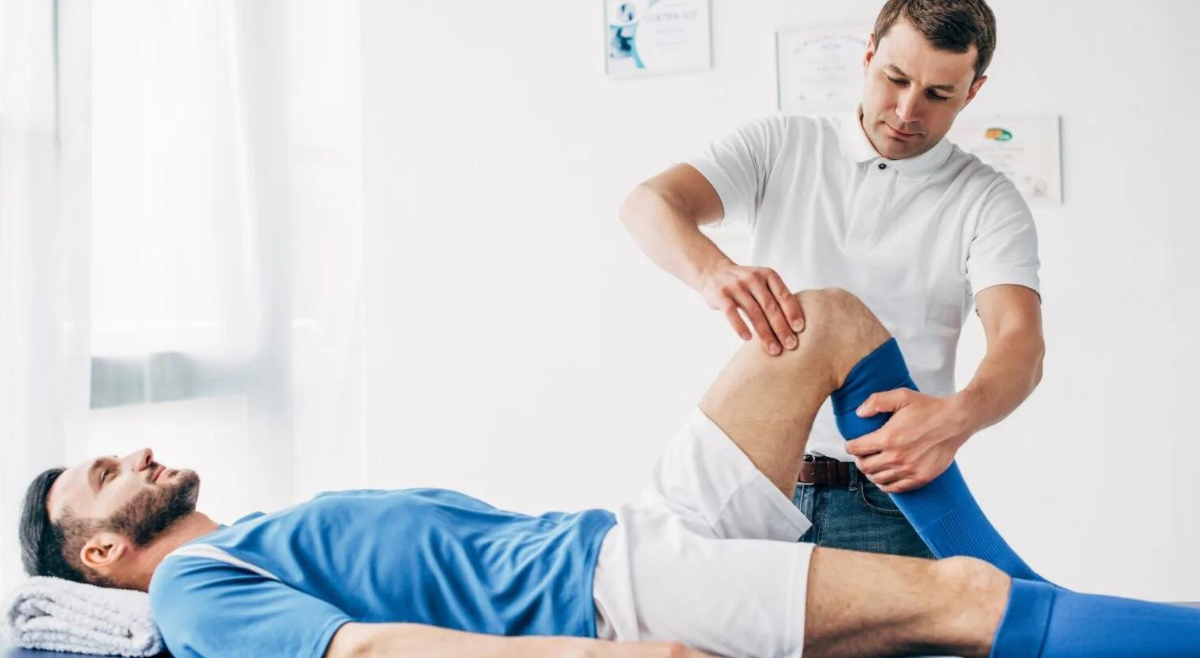
When an injury affects the central nervous system or spinal cord, certain neural connections may be disrupted or lost. Through structured therapy and consistent practice, alternative synaptic connections can emerge to offset damaged areas. This mechanism is known as cortical remapping. Rehabilitation specialists use research-supported interventions such as physiotherapy, occupational therapy, and speech-language therapy to stimulate this restorative process. Repetition, task-specific training, and movement re-education strategies are key components that promote the formation of more efficient brain pathways. Over time, consistent therapeutic exercises can enhance motor skills, cognitive function, postural control, coordination, and communication abilities.
The principle of brain plasticity also plays an important role in neurocognitive therapy. Individuals healing after conditions such as stroke or neurological trauma may face challenges with memory, focus, and executive functioning. Cognitive training programs are developed to support executive functioning and information processing through systematic brain-based activities. Activities that involve attention control, working memory tasks, and analytical techniques help engage underused areas of the brain. As these brain networks are consistently stimulated, they become more efficient, supporting gradual progress in everyday performance and self-sufficiency.
In addition to traditional therapies, advanced clinical technologies are enhancing the application of neuroplasticity principles in rehabilitation settings. Immersive digital platforms, robot-supported rehabilitation, and neuromodulation techniques such as transcranial magnetic stimulation are being incorporated into clinical protocols. These specialized tools provide precise, quantifiable, and interactive ways to deliver repetitive training. For example, robotic useful reference devices can support motor activity to strengthen correct movement patterns, while simulated settings simulate real-world activities that promote functional recovery. Such technologies increase participant engagement and provide real-time performance data, which further supports neural change.
The expanding knowledge of brain adaptability look at here has reshaped how healthcare professionals approach recovery. Rather than focusing only on compensating for functional deficits, rehabilitation now emphasizes restoring function through direct participation and intentional training. Timely treatment, personalized care strategies, and active involvement are essential factors in supporting positive outcomes. By applying the science of neuroplasticity, clinicians can design recovery methods that are grounded in neuroscience and supported by measurable progress. This evolution in perspective offers renewed hope for individuals facing complex neurological conditions and highlights the brain’s remarkable capacity for adaptation and growth.